Looking back at 2017, it was a year where a lot of big shifts happened in healthcare. Political changes, especially in the US and Europe, started to shake things up for global markets. We also saw a lot of talk about how much drugs cost and new ways to pay for them based on results. Plus, technology kept changing how we get care, with more apps, wearables, and digital tools popping up. It was definitely a busy year for trends in healthcare 2017.
Key Takeaways
- Political events, like the US election and Brexit, created uncertainty for healthcare markets worldwide, impacting trade and regulations.
- The high cost of drugs became a major talking point, pushing for more transparent pricing and approaches that focus on the actual value of treatments.
- Digital tools and technology became more common in healthcare, from patient apps and wearable devices to new ways of delivering care like telemedicine.
- Patients started to have a bigger say, with a focus on making healthcare services easier to use and involving people more in their own care and research.
- There was a continued rise in treatments for rare diseases and specialized conditions, though getting these new drugs to patients presented its own set of challenges.
Impact of Political Shifts on Global Healthcare Markets
Well, 2017 was certainly a year where global politics really shook things up for healthcare markets, wasn’t it? It felt like every other week there was some new announcement or policy change that had everyone in the industry holding their breath.
Policy Changes Under the Trump Administration
When Donald Trump took office, there was a lot of buzz, and frankly, some anxiety. Many in the biopharma world breathed a bit easier initially, especially compared to the more aggressive stance on drug pricing from his opponent. But Trump himself wasn’t shy about calling out the industry, famously saying the pharmaceutical sector was "getting away with murder." This kind of talk definitely made waves, and you saw stock prices react. He also talked about shaking up the FDA and bringing manufacturing back to the US, which could have had big implications. Plus, he wasn’t a fan of the Trans-Pacific Trade Partnership, a deal that had potential benefits for market access. If the Affordable Care Act, or Obamacare, got significantly changed, that could have introduced new competitive pressures too. It was a real mixed bag of potential upsides and definite uncertainties.
Brexit and Regulatory Uncertainty in Europe
Over in Europe, the whole Brexit situation was still unfolding, and let me tell you, it created a whole lot of questions. The UK’s decision to leave the EU meant more uncertainty about regulations, how medicines would be recognized across borders, and even things like employee migration and R&D investment. It wasn’t clear if this would lead to higher costs and discourage investment, or if it might actually push the UK to really focus on building its own pharma industry. Populist movements were gaining steam elsewhere in Europe too, raising concerns about the stability of the whole Union. This kind of instability makes it tough for companies to plan long-term.
Evolving Trade Agreements and Market Access
Beyond the big political shifts, trade agreements were also a hot topic. The US, often the first place companies wanted to launch new drugs, was seeing its approach to trade partnerships change. This, combined with ongoing efforts in places like Germany and Japan to implement tougher price controls on new medicines, meant that getting products into different markets was getting more complicated. Countries were also looking for more transparency in how drug prices were negotiated. It really highlighted how important it is for companies to understand the specific market access challenges in each region. The push for new health technologies, like those that help control pandemics, also showed how innovation is key in public health [ce1d].
Here’s a quick look at some of the pressures:
- Drug Pricing Scrutiny: Increased public and political attention on high drug costs, affecting both branded and generic medications.
- Regulatory Harmonization Challenges: Divergent approaches to drug approval and market access between regions, especially with Brexit.
- Trade Policy Shifts: Changes in international trade agreements impacting market entry and global supply chains.
Rising Drug Pricing Pressures and Value-Based Approaches
Okay, so 2017 was a pretty wild year for drug prices, right? It felt like every other headline was about how much medicines were costing, and honestly, it was getting a bit much. People were really starting to question if the prices made sense, especially when you looked at what some companies were charging. This wasn’t just a US thing either; countries all over the world were starting to push back.
Public Scrutiny and Regulatory Response
This whole price thing really put the spotlight on drug companies. You had a lot of public outcry, and politicians were definitely paying attention. Some companies, like Allergan and GSK, started saying they’d try to hold off on raising prices, which was something, I guess. Others, though, were still pushing ahead. It felt like a real turning point where the industry had to start thinking about how it was showing the value of its drugs, not just the price tag.
Emergence of Value-Based Pricing Models
Because of all this pressure, we started seeing more talk about ‘value-based’ pricing. The idea here is that you pay for a drug based on how well it actually works for patients, not just because it exists. Companies like Novartis were experimenting with deals where they’d get paid more if their heart failure drug, Entresto, actually helped people. It’s a complicated shift, for sure, and not every country is on the same page, but it felt like a move towards making sure drug costs were more tied to actual health benefits.
Global Trends in Transparency and Reimbursement
Beyond just the price itself, there was a big push for more openness about how prices were set. Countries like Malta were making it a priority to get more clarity on how drug companies negotiate prices. Germany and Japan were also tightening up their rules on what new drugs would get paid for. It meant that getting a new drug approved and paid for was becoming a much tougher hurdle, and companies really had to prove their worth in each market.
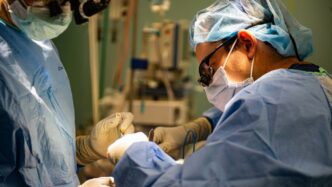
The Digital Transformation in Healthcare Delivery
It’s pretty wild to think about how much technology has changed the way we get healthcare, even just in the last few years. Back in 2017, we were really starting to see things shift in a big way. It wasn’t just about having a website anymore; it was about making healthcare more accessible and personal through digital tools.
Healthcare Apps and Patient Connectivity
Remember when apps were mostly for games and social media? Well, healthcare started catching up. Suddenly, there were apps for everything – tracking your fitness, managing prescriptions, even connecting you directly with your doctor. This made it way easier for people to stay on top of their health without always needing to make a trip to the clinic. This increased connectivity meant patients could be more involved in their own care. It was a big step towards making health information more readily available and manageable for everyone.
Wearable Technology and Real-Time Monitoring
Wearables like smartwatches and fitness trackers went from being cool gadgets to genuinely useful health tools. They started monitoring things like heart rate, sleep patterns, and activity levels. For people with chronic conditions, this meant doctors could get a much clearer picture of what was happening day-to-day, not just during appointments. This kind of real-time data gathering was a game-changer for managing conditions and spotting potential problems early. It’s like having a personal health assistant on your wrist, constantly gathering information that can help improve patient monitoring.
Challenges of Data Integration and Security
Of course, all this new tech brought its own set of headaches. Getting all this different health data to talk to each other was a huge hurdle. Different apps and devices collected data in different ways, and making it all work together in a way that doctors and patients could actually use was tough. Plus, with so much sensitive health information being collected and shared, keeping it all secure became a top priority. Nobody wants their private health details floating around on the internet. It’s a balancing act, for sure, trying to make things convenient while keeping everything safe and sound.
Patient Engagement and Empowerment Initiatives
It feels like just yesterday that healthcare was this thing that happened to you, not something you were really a part of. But 2017 really started to shift that. We saw a big push towards making patients more active players in their own health journeys. This wasn’t just about telling people to take their medicine; it was about giving them the tools and information to really understand what was going on and make informed choices.
User-Focused Interface Design in Healthcare
Think about the apps and websites you use every day. They’re usually pretty easy to figure out, right? Well, the healthcare world started catching on to that. Instead of clunky, confusing systems, developers began focusing on making things simpler and more intuitive for patients. This meant designing interfaces that were easy to navigate, even if you weren’t a tech whiz. It’s like when you’re trying to find a doctor; you want an app that just gets it – finds someone in your area, takes your insurance, and explains things clearly. That’s the kind of user-friendly approach that started gaining traction.
Increased Patient Involvement in Research and Care Decisions
Patients weren’t just passive recipients of care anymore. There was a growing movement to include them more directly in decisions about their treatment and even in the research process. This could mean anything from patients having a clearer say in how their care plan is developed to participating in studies that directly impact the treatments available for their conditions. The idea is that people living with a health issue often have unique insights that can guide research and improve care.
Educational Platforms for Health Literacy
Understanding health information can be tough. You get a lab report, and it’s full of terms you don’t recognize. In 2017, there was a greater emphasis on creating resources that actually helped people understand their health. This included things like:
- Clear explanations of medical conditions
- Interactive tools to track health metrics
- Websites and apps that broke down complex medical data into easy-to-digest formats
It’s all about making sure people have the knowledge they need to manage their health effectively. When information is presented in a way that makes sense, people are more likely to take action and feel more in control.
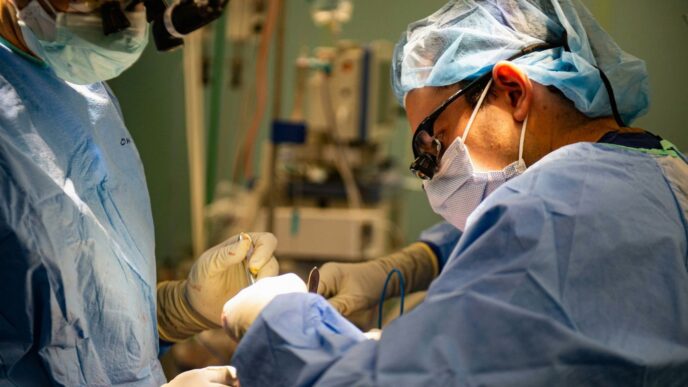
Advancements in Specialty and Orphan Drugs
Growth in Rare Disease Treatments
It feels like every year we hear more about drugs for rare diseases, and 2017 was no different. While the overall number of new drugs approved by the FDA actually went down a bit compared to the year before, a good chunk of those approvals were for specialty treatments. We saw new options pop up for conditions like spinal muscular atrophy and Duchenne muscular dystrophy, which is pretty significant for folks dealing with these tough diseases. It’s a trend that seems to be picking up steam, with more and more companies focusing on these smaller patient populations.
Regulatory Fast-Tracks and Approval Pathways
Getting these specialized drugs to patients faster is a big deal. Because these are often for serious or life-threatening conditions with few other options, regulatory bodies are looking for ways to speed things up. In the US, the 21st Century Cures Act, passed in late 2016, is a good example. It allows for more reliance on things like surrogate markers in clinical trials, which can shorten the development timeline. This is great for patients, but it also brings up questions about how we balance speed with making sure the treatments are truly effective and safe. The debate around Sarepta’s Duchenne treatment, Exondys 51, really highlighted this issue. It got an accelerated approval even though some advisors weren’t totally convinced by the trial data. It’s a tricky balance, for sure.
Challenges of Niche Market Access
Even with all these advancements, getting these high-cost, specialized drugs to the people who need them isn’t always straightforward. The price tags on these treatments can be pretty steep, which naturally leads to more scrutiny from payers and governments. This means companies have to work harder to show the real value of their drugs. It’s not just about getting approved; it’s about making sure patients can actually access and afford these new therapies. There’s a growing need for smarter strategies to manage market access, especially when dealing with these niche markets. Initiatives like the Orphan Drug Access Protocol in the Netherlands are trying to streamline this process for specialized treatments.
Multichannel Communication and Marketing Strategies

It’s getting harder for drug companies to just walk into a doctor’s office like they used to. With all the rules and the sheer amount of information out there, they’ve had to get creative. This means using a mix of different ways to reach doctors and patients, not just one. Think emails, websites, webinars, and yes, still some in-person meetings, but fewer.
Balancing Digital and Traditional Marketing
So, how do you actually do this multichannel thing right? It’s not just about throwing everything at the wall and seeing what sticks. You have to figure out what works best for different people. For example, a busy surgeon might prefer a quick email with key data, while a researcher might want to attend a detailed webinar. The trick is to deliver the right message, through the right channel, at the right time. It’s a balancing act, for sure. You don’t want to overwhelm people, but you also don’t want them to miss out on important information.
Educational Initiatives for Complex Medicines
We’re seeing more and more specialized drugs, especially for rare diseases. These aren’t your everyday pills. They’re complicated, and doctors need a lot of information to understand how to use them and why they’re important. So, companies are putting more effort into creating educational materials. This could be anything from online courses to patient support programs. It’s about making sure everyone involved, from the doctor prescribing the drug to the patient taking it, has a good grasp of what’s going on.
Personalizing Outreach for Healthcare Professionals
Nobody likes getting generic messages that don’t apply to them. That’s where personalization comes in. Instead of sending the same brochure to everyone, companies are trying to tailor their communications. They look at what a doctor specializes in, what their patients need, and what kind of information they’ve shown interest in before. This makes the communication feel more relevant and useful. It’s like getting a recommendation for a book you’ll actually enjoy, rather than a random suggestion. This approach helps build better relationships and makes sure the information gets noticed.
Emergence of New Digital Health Modalities
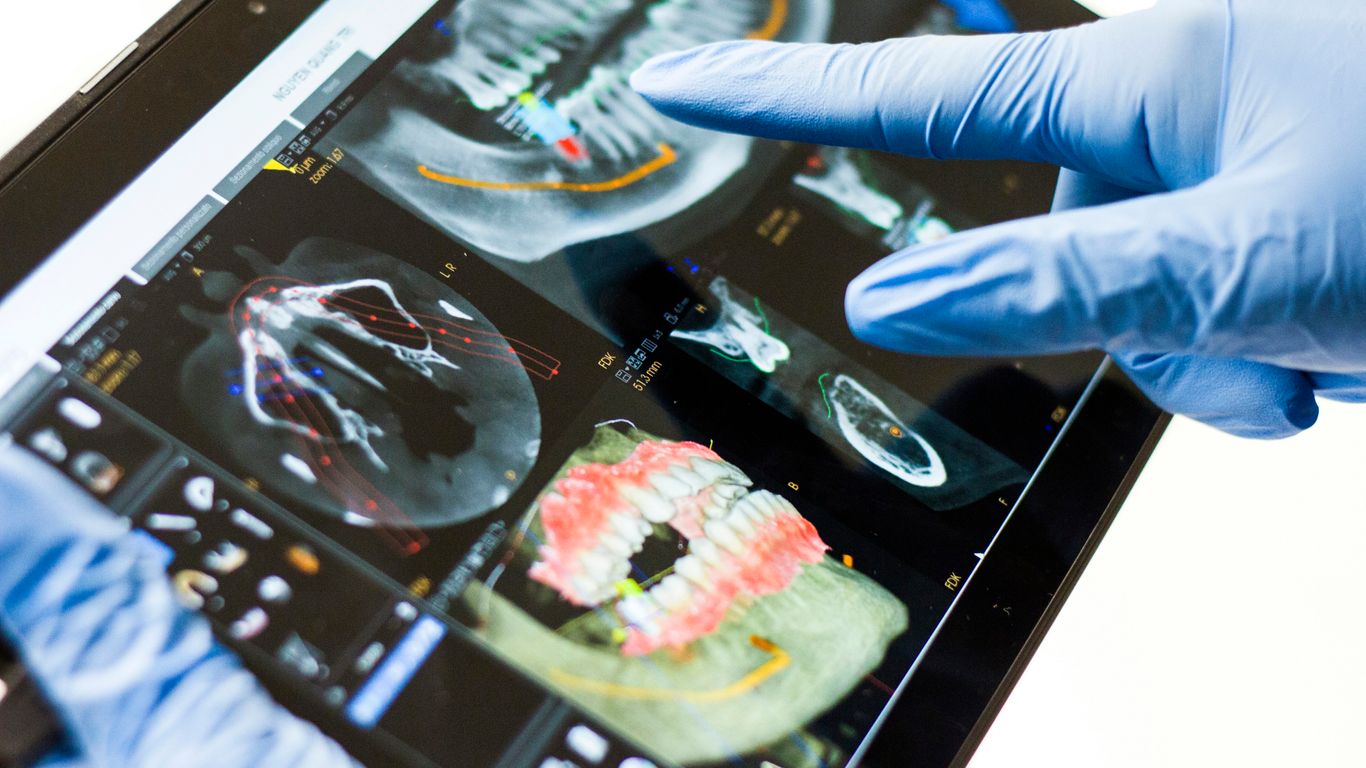
It feels like every day there’s a new app or gadget promising to make our lives easier, and healthcare is no exception. 2017 saw a real surge in digital tools that are changing how we interact with doctors and manage our own well-being. It’s not just about convenience anymore; these technologies are starting to offer genuinely new ways to get care and stay healthy.
Telemedicine Adoption and Accessibility
Remember when seeing a doctor meant taking a whole afternoon off work? Telemedicine is really shaking that up. Being able to connect with a medical professional via video or messaging without leaving your home is a game-changer, especially if you live far from a clinic or just can’t get away. This trend is making healthcare more accessible to a lot more people, which is a big deal. It’s not just for quick questions either; these platforms are getting pretty good at handling actual consultations and even follow-ups. The increasing demand for convenient patient care in today’s fast-paced world has led to the growth of telemedicine and digital health platforms.
Integrating Artificial Intelligence and Chatbots
AI and chatbots are popping up everywhere, and healthcare is a natural fit. Think of a chatbot as a helpful assistant that can guide you through symptoms, remind you to take your medication, or even help schedule appointments. While they won’t replace your doctor, they can certainly streamline a lot of the administrative hassle and provide quick information. It’s like having a personal health guide available 24/7. The goal is to make interacting with the healthcare system less of a chore.
Virtual and Augmented Reality in Medical Training
This one is pretty cool and has huge potential, especially for training. Doctors and students can use VR to practice complex surgeries in a safe, simulated environment. It’s like a flight simulator, but for medicine. Augmented reality (AR) can overlay information onto a patient’s body during a procedure, giving surgeons real-time data. This technology isn’t just for training, though; it’s also being explored for pain management and mental health therapy. Imagine using VR to distract from pain or to help someone overcome a phobia. It’s a whole new way to experience and learn about medicine.
Quality Indicators and System Performance Trends
Looking back at 2017, healthcare systems were closely examined using all kinds of quality indicators. No single data point gives the whole picture, but a mix of measurements helped reveal where things were working, and where they definitely weren’t. Here’s a breakdown of what was tracked and what stood out:
Measurement of Treatment Outcomes
Doctors and hospitals paid a lot of attention to whether their treatments were actually working. The biggest metrics folks cared about included:
- Treatable deaths (people dying from things medical care should prevent)
- In-hospital mortality rates (how often patients didn’t survive a hospital stay)
- Maternal deaths (one of the tougher indicators to stomach)
| Outcome Type | 2015 | 2017 |
|---|---|---|
| Treatable Deaths | 92/100k | 90/100k |
| In-hospital Mortality | 2.0% | 2.1% |
| Maternal Mortality | 21/100k | 18/100k |
The numbers dipped up and down, but the trend was slow. It’s worth noting that population averages can hide big health gaps among different groups.
Efforts to Improve Patient Safety
Patient safety took center stage in 2017. People worried less about rare errors and more about the basics catching patients off-guard, like infections, medication mix-ups, and poor communication. Key focus areas included:
- Hospital-acquired infections (like MRSA and C. diff)
- Medication errors
- How well nurses and doctors kept patients in the loop
Some highlights:
- Most infection rates were dropping until a bump in 2017, especially with device-associated infections.
- 86% of Medicare patients felt staff communicated well on discharge, but only 62% thought the same for medication instructions.
- Hospitals worked extra to clean surfaces and re-train staff, chasing fewer costly mistakes.
US Performance Compared to International Peers
The U.S. liked to say it had some of the best hospitals—but system-wide performance often lagged behind other wealthy countries:
| Indicator | U.S. | OECD Average |
|---|---|---|
| Life Expectancy | 78 | 81 |
| Hospital Readmission Rate | 15% | 10% |
| Preventable Admissions | 19% | 11% |
A few points stick out:
- The U.S. scored high on medical technology access.
- But, patient outcomes weren’t always as good—preventable admissions, for instance, were still way too frequent.
- There was a big push to learn from international systems that put more energy into prevention and better access.
Overall, progress was uneven. Hospitals and providers had short wins, but gaps between the U.S. and its peers didn’t close overnight. Measuring, tracking, and acting on these indicators became the playbook for improvement, even as new problems kept rolling in.
Looking Back and Moving Forward
So, 2017 was quite a year in healthcare, wasn’t it? We saw a lot of changes, from how much drugs cost to how technology is mixing with medicine. It felt like things were moving fast, and sometimes it was hard to keep up. Political stuff, like Brexit and changes in the US, definitely added to the mix, making things a bit uncertain for everyone. But through it all, there was a clear push to make things better for patients, focusing more on what they actually need and experience. It’s clear that the industry has a lot to think about as it heads into the future, especially with all the new tech and different ways people are accessing care. It’s going to be interesting to see what happens next.
Frequently Asked Questions
How did politics affect drug companies in 2017?
Political changes, like those in the US and Europe (Brexit), made things uncertain for drug companies. New rules and trade talks also played a role in how they did business globally.
Why was there so much talk about drug prices?
People were very upset about how much some medicines cost, leading to public complaints and government attention. This pushed companies to think about selling drugs based on how well they worked, not just their price.
How did technology change healthcare in 2017?
Technology became a bigger part of healthcare. Things like health apps, smart watches that track your health, and ways to connect patients and doctors online became more common. However, keeping all this health information safe and organized was a big challenge.
Were patients more involved in their own healthcare?
Yes, patients started to have a bigger say. Websites and apps made it easier for people to understand their health, and they became more involved in decisions about their care and even in medical research.
What was new with treatments for rare diseases?
There was a focus on developing new medicines for rare diseases. Special programs helped speed up the approval process for these treatments, but getting them to the patients who needed them was still tricky.
How did drug companies talk to doctors and patients?
Companies used many ways to share information, mixing online methods with older ones. They also focused on educating people about complicated medicines and trying to reach doctors with messages tailored to their specific needs.