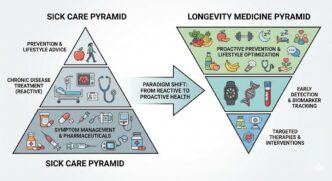
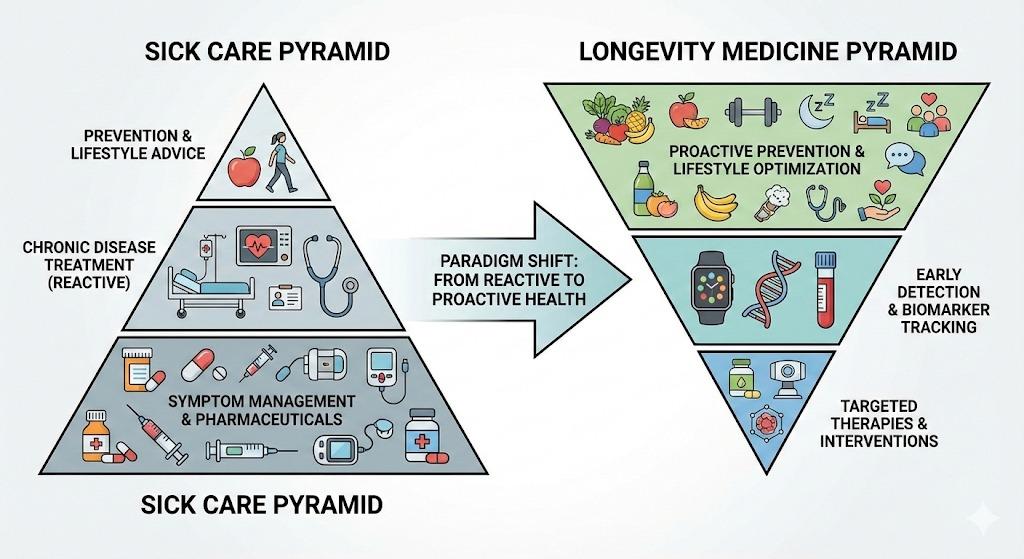
Healthcare in the United States is at an inflection point. Decades of spiraling costs, widening chronic disease prevalence, and uneven preventive care have revealed a stark truth: the system is built to react to illness, not prevent it. That reactive stance is becoming increasingly untenable as scientific insights clarify how disease begins well before symptoms appear and how small perturbations in physiology eventually blossom into full‑blown pathology.
Emerging from this landscape is Longevitix, a preventive care intelligence platform that has introduced its Healthcare Pyramid. This conceptual model reorganizes care around continuous biological insight and early risk detection, rather than late‑stage intervention. The model reframes health not as the absence of disease, but as a continuously measurable and optimizable process.
The Rising Burden of Chronic Disease
Chronic diseases are the principal driver of U.S. healthcare expenditures and morbidity. According to the American Diabetes Association, the total estimated cost of diagnosed diabetes in the U.S. in 2022 was $412.9 billion, with $306.6 billion in direct medical costs and $106.3 billion in indirect costs such as lost productivity.
This reflects a broader pattern: chronic conditions, including heart disease, diabetes, and dementia, now account for roughly 90% of the nation’s nearly $5 trillion in annual healthcare spending.
Despite this economic and clinical burden, preventive care utilization remains inconsistent, with many adults not up to date on basic screenings. Recent CDC data show that in 2023, 69.7% of adults aged 45-75 were up to date on colorectal cancer screening, leaving a substantial portion of the at‑risk population behind.
These trends highlight a fundamental mismatch: disease prevention is known to be cost‑effective and outcome‑improving, yet the system remains oriented toward treating disease after it becomes clinically apparent.
From Episodic Care to Continuous Biological Monitoring
A core limitation of conventional medicine is its episodic nature: patients are seen at annual check‑ups or when symptoms become too urgent to ignore. In contrast, research into digital biomarkers, continuous physiological and behavioral data captured by wearables, sensors, and non‑invasive devices, is accelerating a paradigm shift.
A 2026 study published in NPJ Digital Medicine shows that digital biomarkers derived from wearable sensor data can estimate cognitive and affective states in real‑world conditions, marking early neurophysiological change long before clinical assessments detect dysfunction.
This kind of real‑time, context‑rich health data creates a continuous physiological picture, enabling earlier detection of risk patterns and more precise, personalized interventions.
Inside the Healthcare Pyramid
Longevitix’s Healthcare Pyramid describes a preventive approach that emphasizes measurement, early detection, and targeted intervention. Where traditional healthcare places acute and chronic treatment at the base, and prevention at the narrow top, Longevitix inverts the structure:
- Foundation: Continuous Biological Measurement — The base is built on ongoing, real‑world data captured from wearables, biosensors, molecular diagnostics, and digital biomarkers. Rather than generic benchmarks, this layer focuses on individualized physiological patterns, enabling highly personalized insight into health trends.
- Middle Tier: Early Detection and Risk Tracking — This layer emphasizes longitudinal monitoring and trend analysis. By capturing subtle biological shifts over time, such as changes in metabolic regulation, inflammation markers, or cognitive signal patterns, providers can recognize emerging risk before conventional thresholds are crossed.
- Apex: Precision‑Targeted Intervention — The top of the pyramid is where targeted therapies and clinical actions occur, guided by evidence generated at lower tiers. Interventions are deployed strategically and sparingly, informed by long‑term patterns rather than one‑off snapshots.
This structure reframes healthcare incentives, shifting value away from volume and episodic crisis management toward proactive preservation of physiological stability.
Aligning Systems With Biology
Reimagining healthcare is not only conceptual; it depends heavily on aligning payment models, care delivery, and data infrastructure with preventive objectives. Traditional fee‑for‑service reimbursement, which rewards procedures and visits, often disincentivizes the very early detection and trend tracking that underpin preventive health.
By contrast, value‑based care frameworks and preventive incentive structures encourage investment in screenings, continuous monitoring, and lifestyle‑based interventions.
Likewise, employers and payers are increasingly recognizing the economic opportunity in early engagement: reducing downstream hospitalizations, complications, and disability through sustained risk reduction.
Designing Care Around Human Biology
Longevitix’s Healthcare Pyramid represents a conceptual diagram and embodies a philosophical shift toward health models organized around biology, continuous measurement, and early signal detection. It suggests a future where healthcare is not reactive to crises but anticipatory, using real‑time insights to keep people healthy rather than merely treating them when they are sick.
In this vision, health becomes an ongoing, measurable state rather than an absence of disease. As chronic disease burdens mount and healthcare costs continue to rise, such a preventive architecture, grounded in data, biology, and early action, may prove not just innovative but essential.